by D Knipe
The WHO recognises pesticide poisoning to be the single most important means of suicide globally. Pesticide self-poisoning is a major public health and clinical problem in rural Asia. One approach to reducing access to pesticides is for households to store pesticides in lockable “safe-storage” containers. However, before this approach can be promoted, evidence is required on its effectiveness and safety. In order to provide evidence for effectiveness of these containers we conducted a cluster randomised control trial in the North Central Province of Sri Lanka. A cluster randomised control trial is similar to a clinical drug trial, where a person is randomly given a drug or not. In a cluster randomised trial, we don’t randomise people but instead we randomise groups of people i.e. clusters. In additional for our trial, instead of drugs we gave households “safe-storage” containers.
The Setting
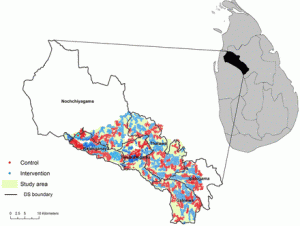
The study population was taken from the Anuradhapura district of Sri Lanka’s North Central province (figure 1). All villages in this area were included unless they had already taken part in pilot studies.
The Trial
The trial had three phases:
- Baseline survey
- Distribution
- Case Detection
Baseline Survey
In order to be able to identify people/households to give a box to we conducted a large census of the study area. We used the 2010 electoral list and Google Earth to identify people to include in the survey. Using a large team of data collectors (A-level graduates) we approached each household to take part in the survey. The interview was conducted as a single face-to-face interview with a household member within the compound of their home. Any household member could provide responses to the survey, but consent was only taken from over 18 year olds.
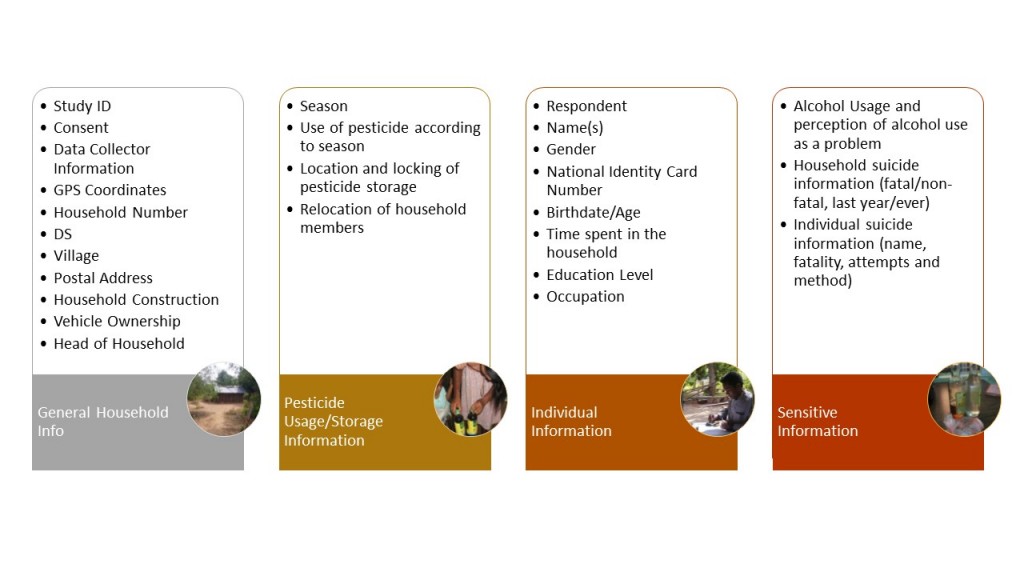
The data collected was primarily entered into a handheld electronic (PDA) device – Juno (figure 2). We collected a range of information (summarised in figure 3). As well as asking questions from the household, we also recorded GPS points for each household included in the survey.
Of all the households eligible to take part in the study 53471 were approached. We achieved roughly a 95% response rate.
Distribution
As this was a large trial including over 50,000 households we staggered the giving out of the Safe Storage boxes. After a certain area of households were recruited to the study (completed the baseline survey) we then identified groups (clusters) of households using the geographic location of households and local knowledge. These clusters were then randomised to either receive the Safe Storage box or not. The Safe Storage device is shown in figure 4.
If a cluster was identified to receive the intervention (box) all households within that cluster who were eligible to receive the box were invited to come collect one at a distribution day (household representative). Households were eligible to receive a box if the household either used/stored pesticides or at least one member of the household was a farmer. At the distribution day an explanation of the device was given (figure 5).
This was followed by a small demonstration on how best to install the device and household representatives given the chance to try the device out (figure 6).
The box was then given to individuals after checking whether they were eligible. Efforts were made to ensure that the boxes were installed in field, compound or house and members of the distribution team followed up in the village to ensure all eligible people received a box.
Case detection
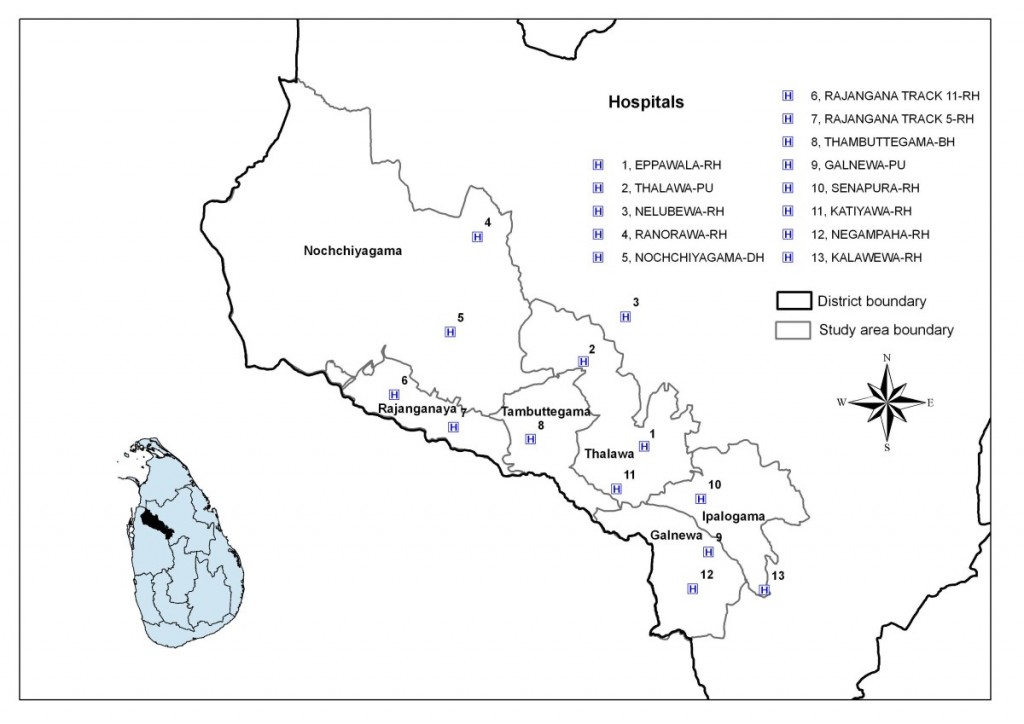
Once households were given a box they were then followed up over a 3 year period and any events of self-poisoning (accidental and intentional) and suicide attempts by any method were recorded. We collected this information by active surveillance of all hospitals in the study area (Figure 7). We also collected information on suicide events reported to coroners. Once collected we then matched these events back to information we collected at baseline. By doing this we will then be able to determine whether the introduction of a Safe Storage device actually does reduce the risk of self-poisoning.
For more information about the trial please read our protocol paper and method paper.